Introduction
The parotid gland is the largest of the salivary glands, located in front of and just below the ear. A parotidectomy is a surgical procedure to remove part or all of this gland, most commonly performed to treat tumours of the salivary glands.
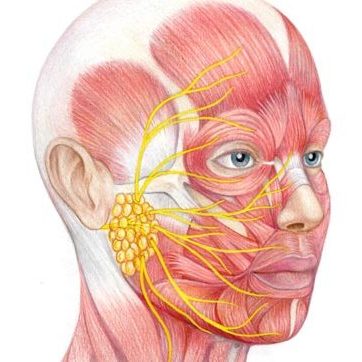
In the head and neck cancer setting, parotidectomy plays a vital role in both removing malignant disease and preserving critical functions such as facial movement. Because the gland lies in close proximity to the facial nerve, which controls facial expression, this surgery requires specialist expertise.
Why Is Parotidectomy Performed?
Common Indications
- Salivary gland tumours – both benign and malignant
- Metastatic head & neck cancer spread to the parotid lymph nodes (e.g. from skin cancers like melanoma or squamous cell carcinoma)
- Recurrent or suspicious lumps requiring removal for diagnosis
Cancer Considerations
- For primary salivary gland cancers, parotidectomy removes the tumour while protecting or reconstructing vital structures.
- For skin cancers of the scalp, face, or ear, the parotid lymph nodes may harbour secondary cancer cells, requiring selective removal.
Types of Parotidectomy
- Superficial Parotidectomy
- Removes the superficial lobe of the parotid gland (the glandular tissues superficial to the facial nerve branches).
- Common for benign or superficial tumours.
- Total Parotidectomy
- Removes both superficial and deep lobes.
- Used when tumours extend deeper or when cancer is confirmed.
- Radical Parotidectomy
- Removes the gland along with part of the facial nerve if cancer has invaded it.
- Often followed by nerve grafting or reconstructive surgery.
Facial Nerve Preservation
A key concern in parotidectomy is the facial nerve, which passes through the gland (separating it into superficial and deep lobes) and controls movement of the face.
- In most cases, the nerve can be preserved.
- If the tumour involves the nerve, part may need to be removed, with options for nerve repair, grafting, or reanimation procedures to restore movement.
This highlights the importance of choosing a surgeon experienced in head & neck cancer surgery, as well as reconstructive microsurgery.
Recovery After Surgery
- Hospital stay: Usually 1–3 nights.
- Drain: is usually placed temporarily to prevent fluid build-up.
- Swelling and bruising: Common around the ear and neck.
- Numbness: Around the ear and jawline is common and may improve slowly over time.
- Return to work: Light duties after 2 weeks, full recovery in 4–6 weeks.
- Follow-up: Patients with malignant tumours may require oncology input for adjuvant radiotherapy or other medical treatment.
Risks and Considerations
- Facial weakness: Temporary or, rarely, permanent (particularly if branches of facial nerve needed to be sacrificed due to tumour removal).
- Numbness: Particularly around the ear and cheek.
- Salivary collection (sialocele): Occasionally requires drainage or neurotoxin injection to reduce the salivary gland activities.
- Frey’s Syndrome: Sweating over the cheek while eating (can be treated if bothersome).
- Scarring: Usually well-hidden in natural skin creases.
Life After Parotidectomy
Most patients recover well and return to normal activities. For those with cancer, ongoing follow-up is essential to monitor for recurrence and ensure optimal long-term outcomes. Reconstructive procedures may be necessary to restore both appearance and function in selected cases.
About Dr Paul Cheng
I’m Dr Paul Cheng, FRACS, a Specialist Plastic, Aesthetic & Reconstructive Surgeon practising on the Gold Coast and in Ballina, NSW. I am frequently involved in management of head and neck cancer – both ablation and reconstruction with microsurgery, ensuring patients receive safe and effective treatment while preserving both function and aesthetics.
📅 Book a Consultation if you have been diagnosed with a parotid gland tumour or head and neck cancer and wish to discuss treatment options.